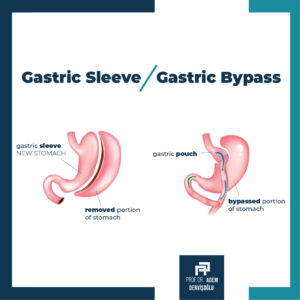
What is Laparoscopic Gastric Bypass Surgery?

Gastric bypass is a combined procedure, providing both volume-limiting and absorption-reducing effects. The first part of the surgery involves the creation of a small new pouch of stomach of about 20-25 ml in volume in the upper part of the stomach. This procedure allows patients to feel satiety after eating small volumes of food. Eating small volumes of food all the time and feeling satiety with these small quantities result in weight loss.
The second part of the operation is the bypass surgery, literally meaning bridging. In other words, the remaining portions of the stomach and some small part of the small intestine are bypassed. This bypassed section will continue to transport the secretions involved in digestion, including the gastric acid, bile, and pancreatic enzymes. The newly formed stomach pouch is connected to a segment of the small intestine located below at a distance of approximately 150-200 cm downward. This way, it is ensured that the food is circumvented farther down the small intestine without going through the rest of the stomach and the bypassed 2 m portion of the small intestine. One effect of this procedure will be canceling the absorption procedure in the bypassed 2 m portion of the small intestine by preventing the gastric content from mixing with the digestive fluids. In other words, some of the food content in the gastrointestinal tract will be eliminated without being absorbed.
Type 2 Diabetes Mellitus (DM) is the comorbid disease associated with obesity, showing the most dramatic improvement after the gastric bypass surgery. It is reported that 82-98% of diabetic patients achieve full remission. Alleviation of diabetes can be attributed to the well-known increased insulin sensitivity effect resulting from weight loss. Thereby, glucose toxicity and lipotoxicity will be reduced and cell functions will be improved.
The restorative effects of the gastric bypass surgery on insulin secretion are followed by favorable changes associated with the intestinal hormones. Ghrelin is a hormone that is likely to have reduced levels after the surgery, the Glucagon-Like Peptide-1 (GLP-1) hormone and Glucose-Dependent Insulinotropic Peptide (GIP) are the classic incretins that stimulate insulin secretion in response to enteral nutrients. After the gastric bypass surgery, the food content in the stomach bypasses the upper parts of the small intestine, reaching the end gut more readily. Following the gastric bypass surgery, the larger postprandial bolus of food in the end gut increases the GLP-1 levels. Since it is an end gut hormone, it starts to reach high levels after the gastric bypass surgery, especially following the food intake. It is suggested that this effect contributes to weight loss.
Gastric bypass surgery is a powerful weapon in your fight against obesity, but it is not a miraculous treatment. Most patients lose 65-90% of their excess body weight in the first year. Gastric bypass also provides excellent results in the treatment of concomitant diseases associated with obesity. These diseases include type 2 diabetes, hypertension, sleep apnea, high cholesterol levels, and acid reflux.
As with all other surgeries, the pace of weight loss may slow down and even weight gain may occur if patients do not follow our recommendations for healthy eating habits and engaging in regular workouts.
Besides the reduction of calorie absorption, the absorption of some important nutrients decreases, too. The bypassed part of the small intestine is responsible for the absorption of calcium, folic acid, iron, and B vitamins. To prevent serious health problems, you should avoid developing vitamin and mineral deficiencies after the bypass surgery. Therefore, you should receive a vitamin-mineral supplementation regimen specifically prescribed for you. This is why it is crucial to attend the follow-up visits and undergo laboratory tests and nutritional counseling after the obesity surgery.